
Perhaps the time-worn expression “having a gut feeling” holds more potency than any of us realized. Studies of the intestinal gut microbiome reveal how disturbances in its biodiversity can affect everything from obesity and autoimmune diseases to chronic depression. As a follow-up to our article the Mediterranean Diet and gut health, we will now delve deeper into the far-reaching effects of gut health and how certified personal trainers can counsel their clients in this area.
What puts the pro in probiotic?
Probiotics are the “good” bacteria naturally found in your gut, also known as live cultures. Their job is to support intestinal health by maintaining a balance of healthy gut flora. Many people are low in this friend-worthy bacteria which is why additional intake of these live microorganisms can be beneficial. Think of it this way: picture your intestines as a war zone, where it’s “good” bacteria vs. “bad”. If the ratio of “bad” bacteria to good is off kilter, this is when tummy trouble stirs. Probiotic consumption acts as the extra armed forces your gut needs to defeat the offending troops and protect the fort from future invaders. Say hello to smooth sailing for your digestive system!
Where are these gut warriors?
Luckily, with the rising popularity of probiotics there a plenty of sources readily available at your local grocery store to choose from. Check these out:
- Yogurt (containing live active cultures)
- Kefir
- Kombucha
- Fermented vegetables (i.e. sauerkraut, kimchi, pickles)
- Fermented soybean products (i.e. tempeh, miso, natto)
- Probiotic Liquid or capsule supplements
What about prebiotics?
Just as it suggests in the name, PRE-biotics come before probiotics, acting as food and fuel for the probiotics. Going back to the war zone analogy in your intestines, think of prebiotics as added ammo your good bacteria need to more efficiently fight off the bad guys. Together, this dynamic duo is your ticket for optimal gut health!
Prebiotics can be found in foods containing fructooligosaccharides, which in layman’s terms is just a certain type of carbohydrate comprised of fructose sugars. These can be found in foods such as bananas, onions, soybeans, whole wheat products, leeks, artichokes, and asparagus. Try pairing some of these sources with your favorite probiotic foods for a tasty and gut-powered meal!
Choosing a Probiotic Product
Word on the street is out and probiotics are hotter than ever! It can a bit overwhelming though when shopping for probiotics due to the surplus of gut-friendly products out on the market right now. So how do you choose the right one? And what’s the best option? In reality, there is no easy answer to this question, as everyone’s body is individualized, especially when it comes to our digestive system. So let’s just start with the most sought-after member of the probiotic family– good ole fashioned yogurt!
Yogurt is still touted by many as the best source of probiotics and for good reason too! As mentioned earlier probiotics are live cultures which means they have an expiration date and can be easily destroyed by heat and an acidic environment. Dairy products are similar in that they have a short shelf life, so you are more likely to consume the probiotics at their highest potency before it goes bad. Plus, dairy foods and probiotics work synergistically—dairy acts as a buffer against stomach acid, increasing absorption of the beneficial bacteria.
Not all yogurt is created equal
Here is what to look for when choosing a probiotic rich yogurt source:
- Contains at least 3 of these strains: Bifidobacterium lactis, Lactobacillus bulgaricus, Lactobacillus acidophilus, Streptococcus thermophilus under the ingredients list
- Reads: “Contains live active cultures” on the container
- 12 gm or less of sugar (you don’t want the sugar to overpower the amount of good bacteria—too much sugar is not beneficial for both gut and overall health)
- Refrigerated—yogurt loses its beneficial probiotic properties when it is exposed to heat which kills the live active cultures (try consuming yogurt fresh out the fridge for increased benefits)
Many people ask what the difference is between Greek yogurt and plain yogurt. The biggest difference you may notice is the texture of Greek yogurt is a lot smoother and creamier than plain. This is due to different processing techniques. Some products strain the liquid whey and lactose from plain yogurt, giving it that thicker consistency, while others add thickeners such as gelatin, corn starch or whey concentrates.
The health pros of Greek yogurt are it contains higher amounts of protein in comparison to plain yogurt, however, the cons are it loses some of its vitamins and minerals such as Calcium in the former process. Keep in mind when choosing the right product for you to look at the nutrition label.
For those who prefer the supplement form or are unable to consume dairy, it’s important to understand what these two terms on the label mean when choosing the right product:
With regard to strains, the different types of bacteria contained within the supplement which each have different benefits and potency (examples of different strains: Bifidobacterium, Lactobacillus bulgaricus, Lactobacillus Acidophilus, Streptococcus thermophilus, B. longum, S. thermophilus) CFU (colony forming units) – the total amount of beneficial bacteria in the supplement —look for ones in the billions range or above
When choosing the right probiotic it may require a bit of trial and error to see which one works best, as all our bodies react differently and each of our guts may be lacking in different strains of healthful bacteria. Once finding a source that does work, your clients will see the reason behind probiotics’ recent claim to fame and their belly will personally thank them for it (and you too for helping them discover it)!
The Gut-Microbiome, Inflammation, and Obesity
Systemic chronic low-grade inflammation, often associated with obesity, renders an individual prone to cardiovascular diseases and type 2 diabetes. Past research honed in on unregulated adipose tissue or insulin resistance as the main culprits in inflammation. However, systemic inflammation involves a complexity only recently studied and still somewhat of a mystery.
Chronic inflammation often presents in individuals consuming a high-fat diet; scientists now posit whether this condition appears as a prelude to obesity-related metabolic disorders, not an end product since the gut microbiome appears substantially different in those living with autoimmune diseases, obesity, and other metabolic disorders.
Considering the human gastrointestinal system receives first exposure to everything we ingest, the supposition exists that as diet affects the gut microflora, systemic inflammation might result. The medical community feels that a promising step rests on the premise that restoring gut microbiota composition (by dietary intervention, prebiotics, and probiotics) could mitigate disease.
High-Fat Factor
To examine the relationship between food consumption and gut dysfunction, a study was conducted with two groups of subjects: one received a high-fat diet, the other continued to consume normal meals. Data revealed that the higher fat diet aligned with significant changes in the gut microbiome, intestinal permeability, and systemic low-grade inflammation. Glucose tolerance also plummeted.
Armed now with the strong conviction that one’s gut microbiome plays a key role in the appearance of inflammation and altered metabolic pathways, future studies plan to assess whether probiotics might serve as an important tool in both the treatment and prevention of obesity and Type 2 diabetes.
Not All Calories are Created Equal
According to a study published in the journal Nature Communications, the human body appears to react differently to calories ingested from high-fiber whole foods vs. ultra-processed or “junk” foods. The latter get absorbed faster upon entering the upper GI tract, rendering fewer calories enter the gut microbiome at the end of the digestive tract.
Conversely, high-fiber foods can remain intact longer, sustaining the full journey to the large intestine. Here, the trillions of bacteria comprising the gut microbiome can begin to get busy. Interestingly, the net result seems a reduction of caloric intake.
The study reveals that gut microbes exist in a perennial tug of war with the rest of the body for calories, said Karen D. Corbin, an investigator at the AdventHealth Translational Research Institute of Metabolism and Diabetes in Orlando and the lead author of the study.
She further adds, “On a Western diet that doesn’t feed the microbes very much, almost all the energy goes to us and very little goes to the microbes. We don’t give the microbes any opportunity to utilize the calories we ate because we use them all. We pull the rope all the way to one end.”
To minimize early absorption and to maximize the quantity of food ultimately reaching the microbes in the large intestine, choosing a diet comprised of whole foods rather than their processed counterparts keeps the gut microflora happy and in peak working order.
Such a meal plan advocates eating whole nuts over nut butter, steak instead of ground beef, and fresh whole fruits as opposed to processed juices. Such a plan ultimately leads to weight and body fat loss, a primary reason clients state for seeking out the expertise of personal trainers.
The Gut Microbiome and Organ Cross-Talk
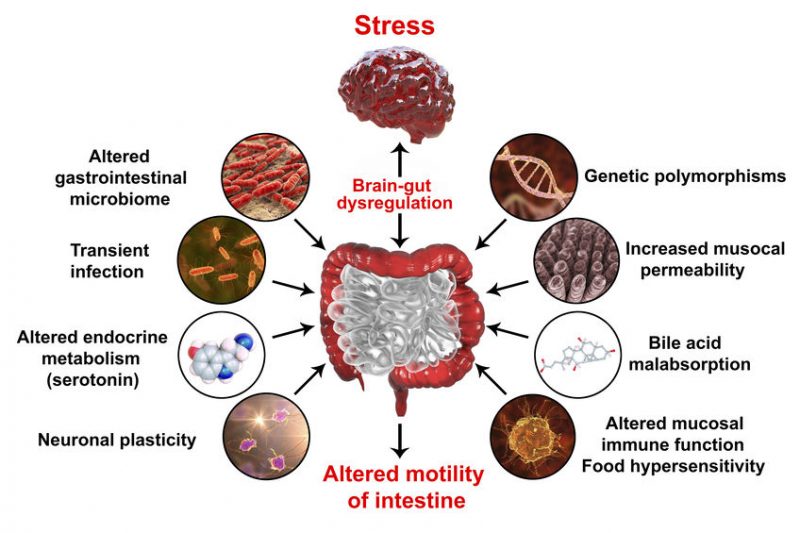
Upon closer inspection, scientists noted the presence of what they call “bi-directional cross-talk” between host microflora and the endocrine system, the point of origin for autoimmune dysfunction. The immune system participates in such cross-conversation.
The gut microbiome not only regulates systemic immunity; the immune system also contributes to the biodiversity of the microflora. This mutual communication between the microbiota and the immune system underscores how the human body’s health relies on “outside-in” and “inside-out” systems of checks and balances.
The ever-evolving studies on intestinal microflora now demonstrate that inflammation within the central nervous system also stems from our gut health. Once again, bi-directional communication occurs, referred to as the “brain axis signaling pathways”.
A healthy gut landscape can transmit brain signals through connections involving neurogenesis, neural transmission, and behavioral control. Disruption to the indigenous gut microbiota renders these pathways dysregulated; the resulting altered permeability negatively affects the blood-brain barrier.
It seems feasible then to see how gut microflora has a powerful impact on mental health, most notably stress, depression, and anxiety disorders. As a prime example, over 20% of individuals living with chronic inflammatory bowel disease suffer from some manner of sleep disturbances and depression.
The “Inside-Outside” Scoop
Clients often open up to us about how they “do everything right” with regard to lifestyle and diet, yet still cannot achieve their goals. Educating them about the far-reaching effects of their gut microbiome could shed some light on their predicament. Trainers have the ability to guide clients, reminding them how healthy insides keep us fit and disease-free.
References:
http://www.todaysdietitian.com/newarchives/100111p46.shtml
http://www.health.harvard.edu/vitamins-and-supplements/health-benefits-of-taking-probiotics
researchgate.net/publication/267456880_Crosstalk_between_intestinal_microbiota_adipose_tissue_and_skeletal_muscle_as_an_early_event_in_systemic_low_grade_inflammation_and_the_development_of_obesity_and_diabetes
pubmed.ncbi.nlm.nih.gov/28968517/
pubmed.ncbi.nlm.nih.gov/28675945/
ncbi.nlm.nih.gov/pmc/articles/PMC7510518/
ncbi.nlm.nih.gov/pmc/articles/PMC6104804/
atlasbiomed.com/blog/link-between-gut-bacteria-and-weight-loss/
pubmed.ncbi.nlm.nih.gov/31547555/
pubmed.ncbi.nlm.nih.gov/31451009/
pubmed.ncbi.nlm.nih.gov/31861086/
https://pubmed.ncbi.nlm.nih.gov/29861127/
https://pubmed.ncbi.nlm.nih.gov/26185088/
https://pubmed.ncbi.nlm.nih.gov/33362788/
https://www.washingtonpost.com/wellness/2023/06/13/weight-loss-calories-fiber-microbiome/
https://www.nature.com/articles/s41467-023-38778-x






