Tensor Fasciae Latae, otherwise known by its abbreviation TFL, is a thin muscle of the hip region located on the thigh just inferior and lateral to the anterior superior iliac spine (ASIS). Despite its small size, the TFL is largely important with a number of functions, including hip abduction, internal rotation, and hip flexion. The muscle gets its name from an additional function: to tense the fasciae latae. Here are the important anatomical functions and implications personal trainers need to know about this muscle.
What is Fasciae Latae?
To understand TFL, we must first explore the fascia.
Fascia is a sheet of fibrous tissue that envelops the body beneath the skin; it encloses muscles and groups of muscles and separates their several layers or groups. The fasciae latae is the deep fascia of the thigh, beginning around the pelvis at the iliac crest and ending just below the knee at the tibia.
At the lateral thigh, the fascia thickens and forms what we know to be the IT band (the iliotibial tract) and encircles the tensor fasciae latae.
TFL Facts and Functions
Key Facts
Origin: ASIS and outer edge of iliac crest
Insertion: Iliotibial tract
Innervation: Superior gluteal nerve (L4, L5, S1)
Hip flexion is considered TFL’s primary function, as it is most active during the acceleration phase of running.
However, its various functions and anatomical positioning make TFL a complex muscle that is both poorly understood and often overlooked when clients consider the source of their pain. This little muscle is associated with four movements in addition to stabilization responsibilities:
At the hip, TFL is involved in flexion, abduction, and internal rotation. Its insertion at the knee via the IT band means TFL is considered a 2-joint muscle and is, additionally, involved concentrically in tibial external rotation.
The TFL is grouped with the gluteal muscles (maximus, medius and minimus) and shares a fascial connection with gluteus maximus as they both insert at the IT band. Together with gluteus maximus, the TFL stabilizes the hip joint and indirectly plays a role in stabilizing the knee by tautening the IT band and bracing the knee when the opposite foot is lifted.
Clearly, TFL does not act alone in any of these functions and we must consider the primary movers and synergistic muscles in any given movement. The other muscles involved in hip flexion are the iliopsoas, rectus femoris, and sartorius; additionally, gluteus medius and minimus are involved in both hip abduction and internal rotation; biceps femoris controls tibial external rotation.
When having to compensate for muscles with overlapping functions that are not doing their jobs effectively, TFL will eventually overpower primary movers and become shortened and hypertonic.
Overactive Tensor Fasciae Latae
TFL has a tendency to be overworked, in part due to its many functions. If gluteus medius (a historically weak muscle) doesn’t do its part in hip abduction, the TFL may be overactive. Similarly, if the psoas is underactive in hip flexion, the TFL will take over. It is not unlikely for someone to simultaneously have a weak gluteus medius, an underactive psoas, and a slow-firing gluteus maximus, in which case TFL is overactive in each of its varying functions.
Because of its connection to the IT band, TFL dysfunction can also contribute to IT band syndrome. In this case, it may present as knee pain or a taut IT band. Since IT band discomfort is such a common complaint and highly misunderstood, we should always consider the TFL in these instances.
A positive Trendelenburg test (hip drop on the contralateral side of a single leg stance) or valgus knees in an overhead squat assessment can both indicate an overactive tensor fasciae latae.
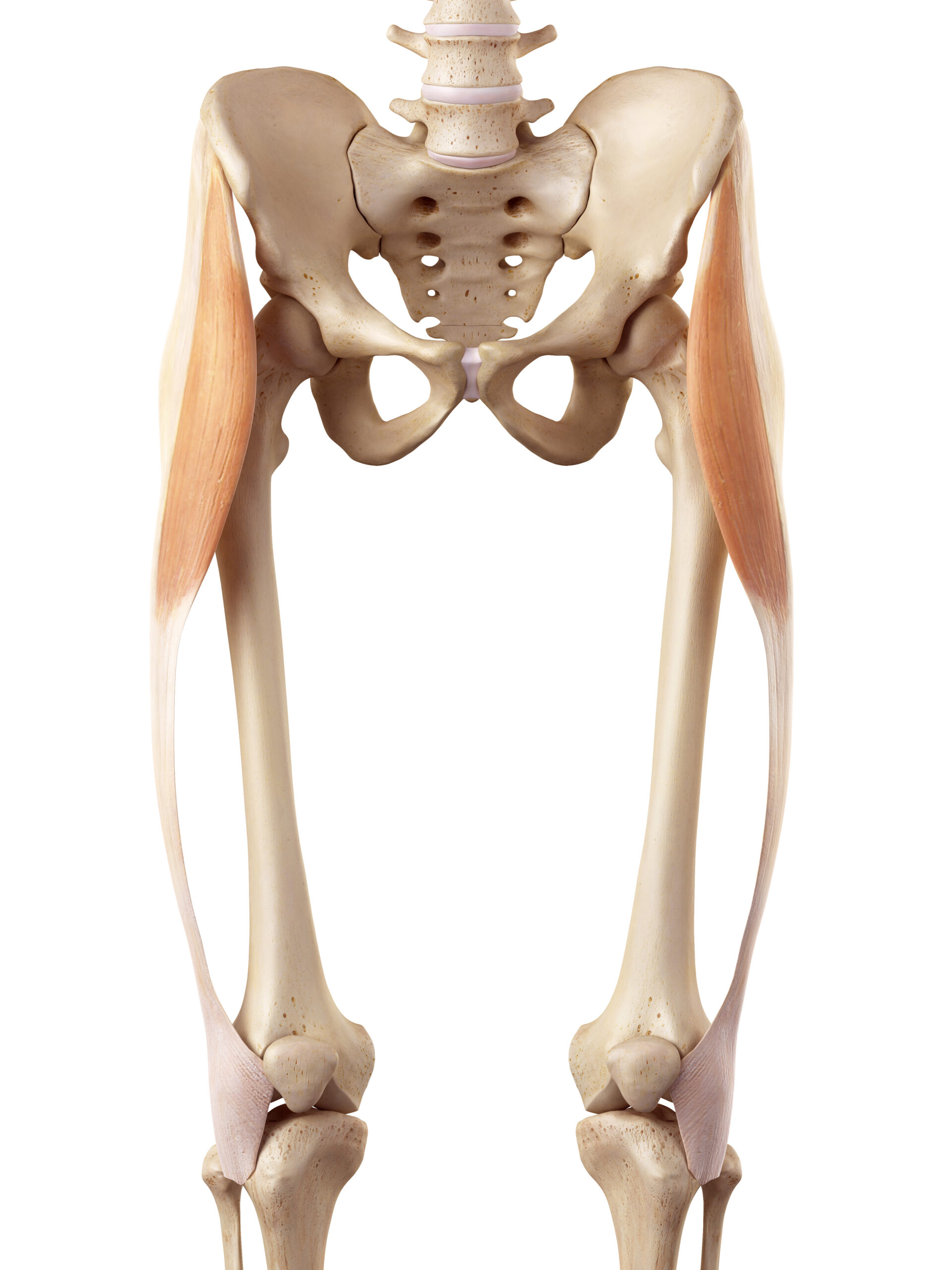
Common TFL Compensatory Patterns
Because it is a 2-joint muscle, an overactive TFL can cause pain at both the hip and the knee.
Compensatory patterns develop from a combination of joint dysfunction and muscle weakness. In the case of TFL, it is most often related to hip joint dysfunction and gluteal inhibition.
For example, during hip abduction, gluteus medius and minimus should fire first followed by TFL, piriformis, and quadratus lumborum. When gluteal muscles are weakened, the brain will often recruit TFL, sometimes in conjunction with piriformis. Over time, this can contribute to sciatic-like symptoms.
Over time, this chronic shortening of the TFL can eventually pull on the IT band and result in ITB syndrome or knee pain.
Minimize TFL Activation
Understanding the compensatory patterns, in order to minimize tensor fasciae latae activation, we must strengthen the primary movers in each of its functions.
TFL Compensatory Motion: Hip Abduction/Internal Rotation
Solution: Strengthen Gluteal Muscles

Because issues with TFL are most commonly related to gluteal weakness or inhibition, strengthening the glutes will most often be the focus. It is difficult to completely isolate gluteus medius and minimus, but studies have shown that resisted side stepping in a squat position minimizes TFL activation and increases activity of gluteal muscles.
To perform resisted side-stepping, place a resistance band at the ankles, assume a squat position, and move laterally.
TFL Compensatory Motion: Hip Flexion
Solution: Strengthen Iliopsoas

A unilateral bridge can be beneficial to strengthen the gluteal muscles of the extended hip and hip flexors of the lifted leg. Unilateral work is helpful in correcting imbalances, including TFL compensation.
TFL Compensatory Motion: Tibial External Rotation
Solution: Strengthen Biceps Femoris
Lying leg curls can strengthen biceps femoris, a hamstring muscle, that is involved in tibial external rotation. Using the machine to perform the leg curl, rather than performing standing hamstring strengthening exercises like deadlifts, can reduce the stabilizing function of TFL. Turning the toes inward slightly will also activate the semitendinosus and semimembranosus involved in tibial internal rotation.
(*For those who have a tell-tale externally rotated tibia at rest when the knee is flexed or that manifests during an overhead squat assessment, these muscles will also have to be strengthened to restore muscle balance)
Release and stretch TFL
Finally, it is helpful to release and stretch the tensor fasciae latae. To release, lie on a massage ball placed directly on the muscle. You can stay there and breathe or gently move to strip the muscle.
After releasing with a massage ball, you can perform a standing TFL stretch.
To stretch the right TFL, stand with the left side of your body facing a nearby wall, and place the left hand on the wall. Move the right hip into extension, bringing the leg behind you, and then into adduction, bringing the leg toward the wall. Step the foot down near the wall and hold the right leg in this position (extended and adducted). Stay for five breaths. Additionally, you could reach the right arm up and toward the wall for a lateral stretch. Repeat on the other side.
Intentional, targeted stretching and strengthening can eventually break this compensatory movement pattern and support optimal, functional movement.
Conclusion
Tensor Fasciae Latae has many jobs and often doesn’t have the support it needs. By regularly massaging and stretching TFL, and targeting the surrounding muscles so that they can step up and do their part, we may be able to help our clients not only to feel better, but to move more efficiently.
[sc name=”anatomy” ][/sc]
References
www.kenhub.com/en/library/anatomy/tensor-fasciae-latae-muscle
fascia. (n.d.) Medical Dictionary for the Dental Professions. (2012). Retrieved January 3 2021 from https://medical-dictionary.thefreedictionary.com/fascia
anatomyzone.com/articles/tensor-fasciae-latae-muscle/
www.sportsinjurybulletin.com/tensor-fascia-latae-unraveling-the-mysteries/
neurokinetictherapy.com/2012/03/15/the-often-overlooked-tensor-fascia-lata/
www.jospt.org/doi/full/10.2519/jospt.2015.5888#.VgVOHLSyMuIwww.noraxon.com/motor-patterns-pathologies-installment-3/
www.clutchpt.com/learn/how-to-fix-knee-pain-by-minimizing-tensor-fascia-latae-tfl-activation
www.precisionmovement.coach/tensor-fasciae-latae-pain-techniques/