“Not having a leg to stand on” is an adage for lacking physical support. Clients may experience physical pains or medical conditions of their lower legs. Certain conditions mandate modifications to exercise and activities of daily life. Others that are more severe may be only remediated by orthopedic intervention. Trainers can support clients’ mobile actions as assurances they do have strong legs to stand on. They should also be aware of “pre-hab” and “re-hab” best practices to prevent lower leg pain.
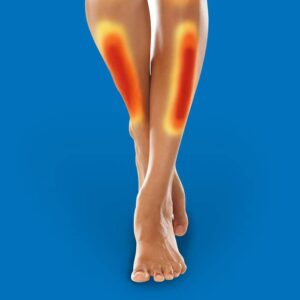
I recently discussed how our ankles and feet normally absorb high dynamic loads transferred to our bones. Moving up a biomechanical chain, our lower legs also absorb impressive static and dynamic loads from weight-bearing activities.
Notes: a. Adaptive protocols are assuredly needed if a client has a “below the knee” or a high leg prosthetic. The balance of this post will address clients that do not wear leg prosthetics. b. Moderate Leg Length Discrepancies (LLD) of more than one inch (30 millimeters) might prescribe surgical intervention. Two added caveats for LLD are “1. Individuals who are on their feet most of the day or who are involved in sports seem to be more sensitive to LLD” and 2. “younger persons, on the whole, are able to adapt to larger LLD than older persons.” (1).
Potential for Lower Leg Injury
Life can go wrong in a “normal” locomotion or in a dynamic workout. Consider how a client steps off a curb, or makes an exercise plyometric move, or jogs on a sloped beach, or increases running distances too quickly over time. Excess or chronic stresses on our muscles, connective tissues and bones can, at times, go wrong. And LLD can exacerbate such instances for our lower legs.
According to one National Institute of Health report, Hospital Emergency Rooms or Urgent Care facilities address 15 million cases of lower limb strains, pains, and sprains annually (2).
- This article cites the four compartments of a lower leg as context for potential overuse or trauma conditions.
- It then addresses three prevalent conditions or injuries which clients may experience in their fitness journeys.
- Prudent “pre-habilitation” or preventative actions are cited for those top 3 problems, as “re-hab” may unfortunately take several to many months for recovery.
- Key takeaways will help Trainers enable best possible mobility for their clients, factoring gender, age and exertion levels into their recommendations for safe and effective training.
Four Compartments
Our lower legs (regionally from our knees to our ankles) can be physically described in four (4) longitudinal compartments that are separated by fascia and adjoin the tibia and fibula bones.
Each of these lower leg compartments can cause either acute or chronic pain when something goes wrong.
- Anterior (along the smaller tibia bone and connecting to toes)
- Anterior Tibia Syndrome can develop in this region after sudden strenuous exercise or long hikes.
- Lateral (distal and connecting to the heel and underside of foot)
- Acute or chronic pain in this compartment can be generated by swelling of the lateral muscles that rub against fascia.
- Deep Posterior (backing the fibula and connecting to the side and lower parts of a foot)
- A client may sense needles and pins or numbness in a foot or have deep aching pains in the leg. These compartment pains may suggest medical attention when the deep calf muscle has swollen significantly.
- Superficial Posterior (the largest compartment that connects to the heel/calcaneus foot bone).
- Pain here may be caused by anterior/posterior muscle imbalances, or other causes.
About a third of athletic injuries to our lower limbs are strains or sprains (2). These injuries can often be self-administered with classic “R I C E” treatments (and non-prescription painkillers) or done under a medical professional’s observation.
- Rest
- Ice (for the first day or two after trauma)
- Compression
- Elevation.
[sc name=”running” ][/sc]
Three Priority Medical Conditions or Injuries of Lower Legs
Three lower leg conditions or injuries that can be more severe and longer-lasting are:
1. Shin Splints, with 3 million reported cases in the USA annually (3) and Stress Fractures:
The National Athletic Trainers’ Association and American Academy of Orthopedic Surgeons provide an information-rich online infographic for key Facts, Diagnoses and Prevention of Shin Splints or resultant Stress Fractures.
Shin splints are acute or chronic pains in a ~5-centimeter region along one’s tibia. “Medically known as medial tibial stress syndrome (MTSS), shin splints often occur …after intensified or changed training routines (3)” thereby taxing lower leg muscles, tendons and bone tissue. If training is not relaxed, the painful area may become stress fractured.
Half of all diagnosed stress fractures occur in our lower legs.
Female athletes may experience these fractures more than males.
2. Achilles Tendinopathy is a fairly common “overuse” injury for about 200,000 persons each year. An acute extreme for this lower leg tendinopathy is a rupture that can sideline a client for many months of pre-hab, intervention and rehabilitation. Some studies suggest that Achilles Tendinopathy is more prevalent above the age of fifty.
3. Deep Vein Thrombosis (DVT). This type of leg pain can be life threatening yet is not always easy to diagnose. Who is most susceptible to potentially dangerous clotting in lower legs?
-
- Those over the age of 40, and males at higher incidences than females
- Those with a family history, or having had a prior blood clot
- Those who are inactive, or who sit for long periods – like knowledge workers or air-travelers.
- Overweight or obese clients
- Clients who suffer a major injury.
A Big Deal? Yes, as one-tenth of all DVT sufferers experience pulmonary embolisms.
Preventative Steps and Modifications
When clients experience “minor” leg pains that are not muscular soreness or delayed onset of muscle soreness (DOMS), trainers may recommend modified motions and add special stretches to keep clients moving with manageable discomfort. If lower leg pains are diagnosed by medical professionals as more than muscle fatigue, trainers should evaluate the client’s exercise trends and potential for overtraining that may lead to compartment syndromes, or the more serious conditions described above.
Certain competitive clients may try to press on through lower leg discomforts or pains that are not muscle fatigue. Remediations like these may be suggested,
- Analyze athletic shoes for pronation or supination wear
- Recommend level and soft walking or running surfaces
- Establish limitations to the volume and intensity increases of weight-bearing motions
- Ten percent (10%) increases are prudent benchmarks for distance escalations per week.
- Reduce repetitive stresses by cross-training
- America’s Olympic Medalist and Boston Marathon Winner, Meb Keflezighi, cross-trained on an elliptical trainer and wore “high” compression socks* in his impressive volume training
- Establish longer periods of post-exercise recovery
- Suggest focused flexibility and strength moves to improve muscle imbalances and stability.
*For clients that sit or travel significantly, compression hosiery is often a practical solution for swollen lower limbs and DVT avoidance.
Physical Support Summary
Statistics cited in this article show that lower leg pains and conditions are quite common.
Professional trainers should be mindful that shin splints can lead to stress fractures, and that “training through” leg pain is an unsuccessful approach for remediation. Clients should always be mindful of non-DOMS pains that may need professional medical attention.
Encourage clients to listen to their body’s feedback for both acute and chronic pains so that they can still “have legs to stand on.”
References
- Khamis S, Carmeli E. A new concept for measuring leg length discrepancy. Journal of orthopaedics. 2017 Jun;14(2):276. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5376249/
- Lambers, Kaj et al. “Incidence of patients with lower extremity injuries presenting to US emergency departments by anatomic region, disease category, and age.” Clinical orthopaedics and related research vol. 470,1 (2012): 284-90. doi:10.1007/s11999-011-1982-z.
- Shin splints – Symptoms and causes – Mayo Clinic