We certified personal trainers can be resourceful listeners and agents to help our older clients address both pain dimensions (yes there are two: sensory and emotional). Pain comes from the Latin word poena meaning penalty. A later French word derivation is suffering, as this older gentleman is apparently experiencing in Figure 1:
“Pain is an experience with both sensory and emotional dimensions.”
Ref: OXFORD Handbook of Pain Management
Is Pain all Penalty and Suffering?
No. Despite that word origin of pain, it would be hard to function as a living thing without pain as feedback to our brain. As stated in Pain Science, “There is no pain without brain. “
Although mystifying, inconsistent, and erratic, pain is a “normal” nervous system signal that suggests our body is entering or is already in a danger zone. Painful sensations are responses to perceived and/or actual challenges to our bodies or minds.
For example, a client is attempting a personal best for an open-chain Bench Press. She or he experienced a twinge in the rotator cuff area. That twinge, whether discomfort or worse, is a signal to cease the repetitions to avoid injury. Ignoring such signals is how client pain leads to greater difficulties.
Chronic and Acute Client Pain
The two broad categories of pain are chronic and acute pain.
Chronic pain of any perceived or genuine severity are long-lasting sensations of many months or years.
Acute pain is episodic or short-lived after the cause is eliminated or accommodated. You may hear that a client has undergone “safe” botox injections or electrical nerve stimulation to decrease acute pain. As you may suspect, these formal medical treatments are not 100 percent effective.
Paining Percentages
Rare is the older client who does not experience (or share) one or more of these categories of chronic pain:
Figure 2. Percentage of older Americans who suffer from chronic pain conditions
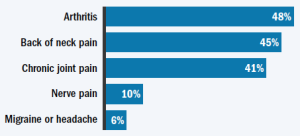
Adapted from Journal of Pain Research, Nov. 1, 2017, pp. 2525–38; Vital Health Statistics, Feb. 2014, pp. 1–161.
Each of these painful conditions in Figure 2 could merit its own complete discussion. We know of many more types of sensory pain. As evidence of the depth and breadth of pain as a wellness and aging topic for millions of clients, the Cleveland Clinic cites many pain management resources which you can find below in the reference section.
Arthritis
As suggested by the bar graph in Figure 2, we are likely to meet and train clients with one or both major categories of Arthritis, which the non-profit Arthritis Foundation suggests is “joint pain or disease.” Joints may be painful, swell in size swelling, and/or cause decreased ranges of motion which impact clients’ activities of daily life (ADL).
- Osteoarthritis. “Osteo” (OA) problems are caused by wear and tear of joints and their connective tissues.
- Rheumatoid Arthritis. Rheumatoid Arthritis (or RA) is an auto-immune deficiency in which inflammation causes joint degradation. It is so weird yet sadly true that our bodies can put our own body parts under attack. Note that one painful condition of some client’s extremities, GOUT, is a separate category of arthritis.
Client Pain and Activities of Daily Living
Some nervous signals to our brains stem from ADLs, as shown in Figure 3 below.
Figure 3: Back Pain and Backaches from ADL – pictogram.
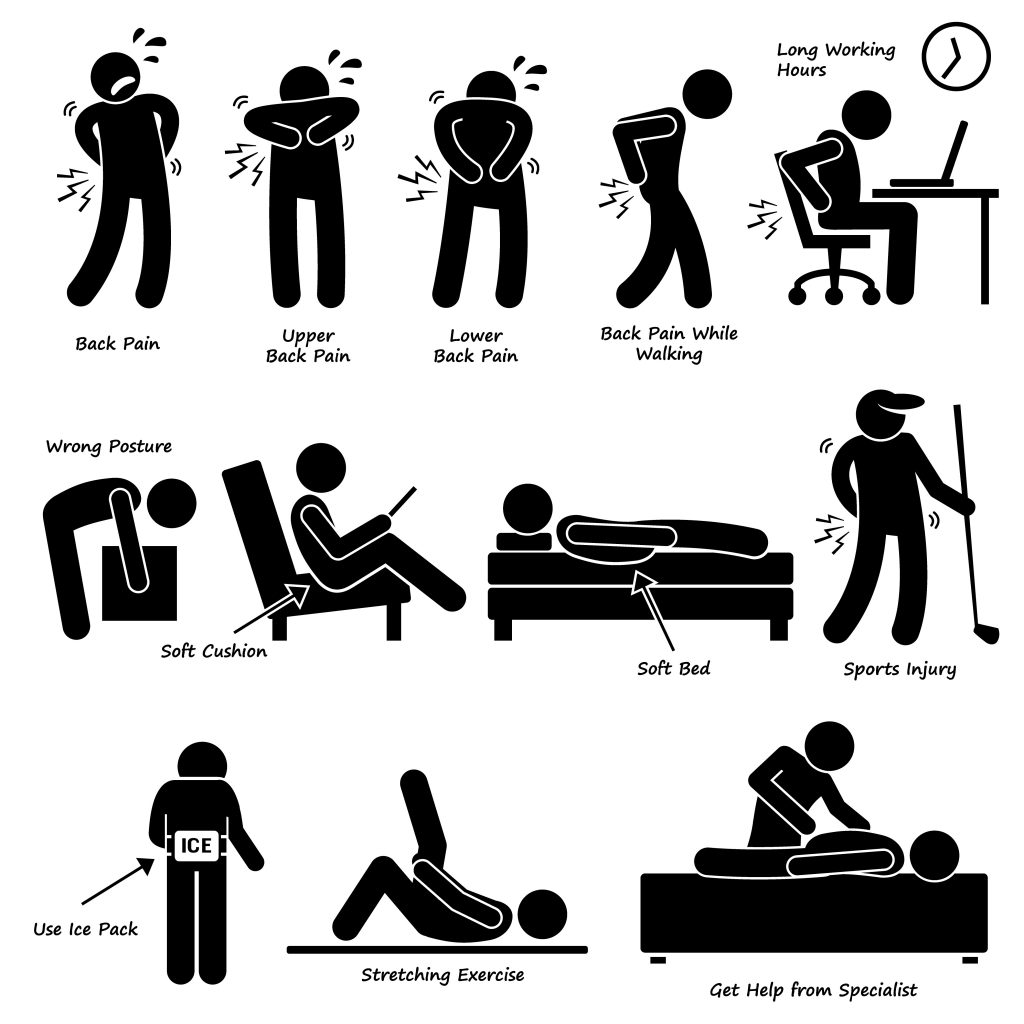
Note three remediations in the bottom row: 1. Ice, 2. Stretching, and 3. Physical therapy.
This painful overview of what our brains receive as precursors to danger helps reinforce the need for formal PAR-Q completion and updates for older clients. It also reinforces the need for continuing education about pain mitigation. It is well documented that actual, or imagined hugging or intimate contact generate a happy “hugging” hormone called oxytocin. What CPT doesn’t want a client to feel happy, and possibly reduce levels of acute pain?
This rhetorical question raises the issue of prescription and non-prescription painkillers for clients. Trainers should always be aware of prescription and non-prescription (ex: NSAIDs) medications that a client is using. Massages, self-myofascial release (SMR) efforts, and physical therapy (as shown in Figure 3 above) are just three non-opioid alternatives to reduce the discomfort, pain, and suffering of clients. Some may choose to seek treatment for chronic pain from a naturopathic doctor. Others may explore other more complicated interventions such as stem cell and PRP treatments.
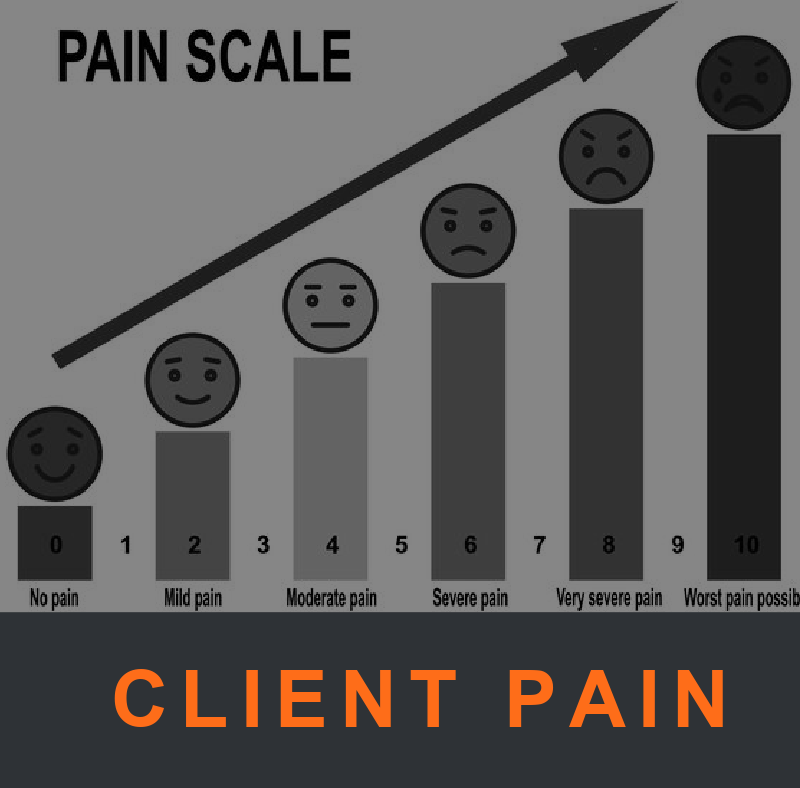
Nerve pain associated with conditions such as sciatica can often be alleviated by performing nerve glides. Certified Personal Trainers should listen, ask sensory questions, and regularly gain subjective assessments of client pain, with verbal feedback or by a client’s choice of a scalar value from this Pain Assessment scale in Figure 4 below.
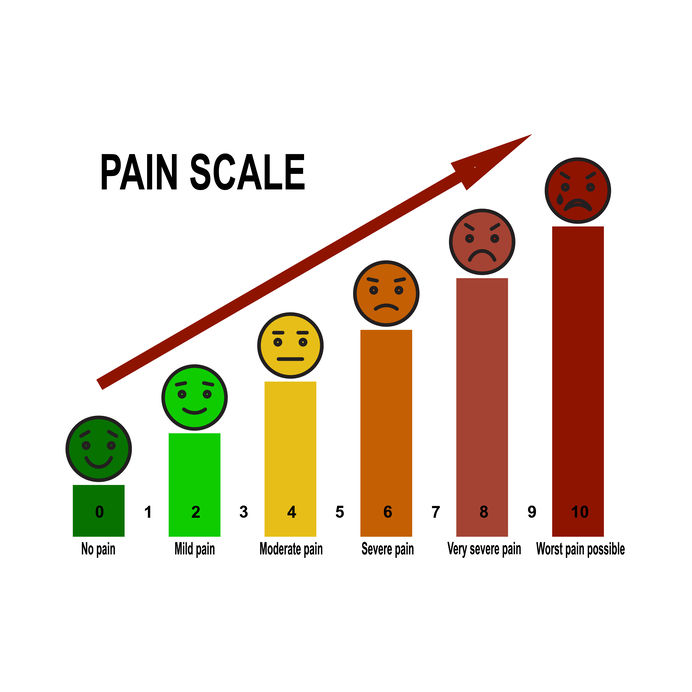
Figure 4. Subjective Pain Assessment Scale for Clients
Copyright: liluydesign Pain scale 0 to 10 is a useful method of assessing pain.
Another example: An older active client who is an active jogger reports episodic (acute) pain in the heel areas of both feet. A trainer can propose interventional alternatives to jogging which may alleviate those pains, still enabling gains for desired stamina. Swimming or other low impact activities are suggested in this case.
Furthermore, runners who experience pain while running may be suffering from a muscular imbalance that has lead to inflammation or tension. Lower extremity dysfunction can be assessed by a qualified trainer to determine if there are corrective exercises that can be done to rebalance posture. When pain is present, this effort should be coordinated with a qualified medical professional.
Summary
CPTs should be prepared to address both physical and mental considerations for prevention, mitigation, and/or remediation of pain with each individualized training program. Anything that can help relieve the pain and keep it under control should be considered, and fortunately there are many options available besides prescription medication.
References
- American Chronic Pain Association (ACPA) www.theacpa.org/
- American Academy Pain Medicine (AAPM) https://painmed.org/aapm-news/american-pain-society
- Arthritis Foundation https://www.arthritis.org/
- Facial Pain Association https://fpa-support.org/
- The Foundation for Peripheral Neuropathy (TFFPN) https://www.foundationforpn.org/
- National Cancer Institute (NCI) https://www.cancer.gov/
- National Fibromyalgia Association http://www.fmaware.org/
- National Headache Foundation https://headaches.org/
- Neurofibromatosis Network https://www.nfnetwork.org/
- National Multiple Sclerosis Society https://www.nationalmssociety.org/
- National Organization for Rare Disorders (NORD) https://rarediseases.org/
- Interstitial Cystitis Association https://www.ichelp.org/
- Reflexive Sympathetic Dystrophy Association (RSDSA) https://rsds.org/
- United Cerebral Palsy (UCP) https://ucp.org/






