In fitness, we not only cater to clients with postural dysfunction but we begin to notice it more in those we encounter in everyday life. You may have older clients who have a “hunchback” or mention a pain in the neck. Or, do you see evidence of spinal misalignment consistent with “text neck“?
Chances are that many clients will lean into a costly remedial condition at some point. “Americans spend about $7 Billion (average) on treatments for neck and lower back pain – more than they spend to treat diabetes or heart disease. Our longevity and our lifestyles are root causes for the high rates of neck and back pain.”
Does a noted Forward Head Posture (FHP) impact your elder client’s range of motion and/or activities of daily life? If not now, is it only a matter of when and what should a trainer do?
- This article reviews known causes, issues, and knotted neck problems that our clients may experience with aging, or aggravate with poor ergonomics at home, work, or play… It builds on prior NFPT posts about FHP and this neck region’s important biomechanics.
- It refreshes our trainer toolkit to assess client posture and recommends stretching and resistance exercises to prevent or mitigate both postural problems of FHP and resultant pain.
- It concludes with a trainer call to action to anticipate and hopefully prevent/mitigate/remediate Neck issues that may diminish a client’s activities and qualities of life.
All About the Neck
A neck is simply yet importantly the connecting region between one’s head and body. Bad outcomes are bound to occur when bones, muscles, connective tissues, and nerve pathways in this region are inflamed, misaligned, or degraded due to one’s age or lifestyle. This complex kinetic and sensory area is supported by many deep and superficial muscle groups, as suggested by this graphic:
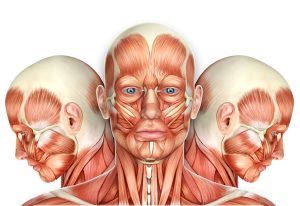
Our long Vagus Nerve (Cranial Nerve #10) passes through this area with its vital sensory and mobility messaging.
Our Accessory Cranial Nerve (#11) controls our neck muscles – permitting us to rotate, flex, and extend our neck and shoulders – without discomfort under good conditions. Certainly one’s head, neck, and shoulder alignment or misalignment impacts one’s neuro-muscular messaging.
The Negative Impact of Forward Head Posture
Each client’s neck region is “shaped” in part by genetic influences and aging. Either or both factors impact a client’s chances of acquiring FHP. With every measured inch of head-tilt forward, our spine absorbs an added 10 pounds of strain. Over time this added stress on the cervical spine will inevitably degrade disc space and potentially lead to severe dysfunction.

Surprisingly, a client’s “gut” may become agitated from FHP. The poor alignment associated with faulty neck posture may interfere with digestion.
FHP can notably degrade a client’s standing balance which may lead to costly (in more ways than one) falls. Falling may be exacerbated by other aging factors like lesser vision or loss of hearing.
Finally, some elders, particularly women over age 70, may develop an auto-immune deficiency named polymyalgia-rheumatica, or PMR, which may lead to chronic, regional muscle weakness or stiffness in the shoulders and neck.
According to the Arthritis Foundation, this inequitable PMR deficiency may be linked to the client’s:
- Fatigue
- Fever
- Poor appetite
- Weight loss
Call to Action
If warranted, professionally address a client’s lifestyle and/or counsel the client about age’s effects on spinal alignment.
If screen (a.k.a. “Tech”) time is an FHP factor, encourage the client to re-assess ergonomics of distance, view angle, and encourage rest intervals. One’s awareness of “tech” ergonomic issues may help a client adapt with better human factors in mitigation efforts.
Perhaps providing a visual of one inch of head tilt adding 10 pounds of spinal and muscular strain could serve as a client’s call to remedial action! Should FHP reach three inches of anterior tilt, the neck and shoulders are strained by supporting the equivalent of a 42-pound bowling ball on top of their shoulders!
Should an elder client share, or if you that a client has trending fatigue, poor appetite, or weight loss, then encouraging the client to visit a medical professional is prudent. PMR, like an immune deficiency, should be ruled out or addressed with bespoke remedial exercises.
Trainers can assist in both preventative and remedial cases of adhesions and trigger points in the neck to ameliorate the postural distortion. Using a foam roller can be helpful for a client to help release muscles at the cervical spine junctions. But it may behoove a client with severe dysfunction to see a qualified manual therapist.
Neck region stretching in all three planes of motion is a fine starting point for most clients, with cervical vertebra fusion as one exception.
- We should remember that the shoulder girdle and upper back may contribute significantly to reported or observed neck issues. Muscles in and around the shoulders and back may become long and weakened, particularly the cervical flexors, or conversely shortened and overactive, such as the intrinsic muscles of the back, as contributors to client neck issues.
If functional assessments lead a trainer to recommend strength moves to alleviate some neck issues – either or both isotonic and isometric exercises may be appropriate.
Summary
Our body follows our head. Thus, trainers must be aware of weakness and spinal alignment symptoms and issues for their elder clients. Genetics, age, and lifestyle cognizance should alert the fitness professional to possibilities of neck knots plus frustrating and distressing conditions like FHP and PMR.
Proactive and tailored stretching and strength regimens for neck, shoulder, and back regions may help older clients maintain their activities of daily life.






