
The Human Heart: we all have one, but how fully do we understand their function? How necessary for certified personal trainers is this understanding to developing an effective training regimen? I believe very, and if you believe athletic development is a scientific discipline, you probably do too. A solid grasp of cardiophysiology can provide fitness professionals the knowledge to critique fad training regimens, program tailored exercise routines, and properly gauge our clients’ work intensity. This is what we’re really paid for- our time developing efficient and effective routines to improve the lives of those who take on this journey with us.
Basic Heart Anatomy and Physiology
The heart has three layers of tissue: the epicardium, pericardium, and myocardium. As personal trainers, we’re most concerned with the myocardium as this is the muscular layer of the heart that is responsive to training.
From here, the myocardium controls four different chambers, which can be broken down into two smaller categories of atriums and ventricles. If we were to imagine the heart as a square divided into 4 sections, the top two chambers would be the atriums and the bottom two chambers would be the ventricles. A trick to remember this is imagining the alphabet starting at the top: A (for atrium) is above V (for ventricle).
The atria act as an entry-reserve for the ventricles. They take in blood and pump it into the ventricles, then some passive filling occurs as well from the atria to the ventricles. The right ventricle will then eject this blood into pulmonary (referring to the lungs) circulation for oxygenation and the left ventricle will push the blood into the systemic circulation that powers our muscles, digestion, and brains, depending on which ventricle we are referring to.
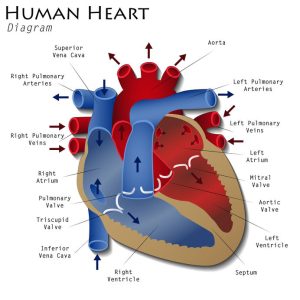
The first stop for deoxygenated blood is the lungs, which houses the vascular system that allows for oxygen and carbon dioxide exchange. This is the one instance in which the arteries carry deoxygenated blood away from the heart, and oxygenated blood returns in the veins to the heart.
Within this vasculature system, things like fluid volume and vascular resistance (the resistance that must be overcome to create blood flow) matter. For example, when the left ventricle begins to fail, this results in a backlog of fluid causing congestive heart failure. When the resistance in vasculature is too high, pulmonary hypertension may result, causing symptoms like dizziness, chest pressure, etc.
We know that exercise could greatly benefit the heart and vasculature for those who are healthy and prevent pathologies like these from developing, but there is also some research that shows moderate exercise could reduce the effects of pulmonary hypertension. If you decide to take on a client with a known pulmonary hypertension disorder, ensure that you adhere to the clearance guidelines laid out by the client’s physician.
In the lungs, the blood is reoxygenated in the alveoli and pushed back into the heart by the flow of fresh deoxygenated blood that is coming in for the exchange process. The push occurs in the pulmonary vein where the blood enters the left atria. This blood is then pumped into the left ventricle with a little bit of downtime for some passive filling to occur, referred to as the atrial kick. It accounts for upwards of 30% of your total cardiac output. This blood is then ejected into the aorta, which has an immediate return to the coronary arteries so that it may obtain the freshest, richest oxygenated blood, then the rest is routed to the body.
The Importance of the Atrial Kick
An important note regarding the atrial kick: it is reduced when the heart begins pumping too fast. So on top of the oxygen that is being depleted in the muscles, they are also not being replenished with as much blood. This lower blood flow also diminishes the removal of other anaerobic respiration byproducts, such as lactic acid.
Clients who may be required to perform under conditions required extended demands could benefit from extended cardio leading to anaerobic exercise.
It’s Electric
Finally, we’ll touch on the electrical system of the heart that makes all this possible. Cells, including cardiac cells, internalize their negativity and push positively charged protons outside themselves to create a gradient (the electrical potential that acts on an ion to drive the movement of the ion in one or another direction).
Cardiac cells are unique in expressing what is referred to as automaticity. This allows a single cardiac cell to depolarize and trigger the depolarization of the cells around it. This occurs uniformly in the healthy heart starting at the top of the right atria in what is referred to as the sinoatrial (SA) node. The important piece to remember is that this process uses positively charged ions like sodium, potassium, and calcium (also known as electrolytes!) to regulate itself and cause contraction and relaxation (referred to as systole and diastole). Hence, the importance of replenishing electrolytes throughout and after long, strenuous workouts is underscored.
Key Points
The important things to take away from this overview:
- Cardiac output can be negatively impacted by a high heart rate due to loss of passive filling time for the atrial kick; again, this accounts for up to 30% of your total blood volume.
- The heart is a muscle and as such has similar metabolic needs as skeletal muscle- we let our major muscle groups rest in between sets to allow recovery to occur, and a similar process (depending on goals) may be beneficial in the efficient training of cardiac tissue.
- In the presence of oxygen, the heart is used as the terminal electron acceptor in cellular respiration, which produces the most energy and allows for the most growth (Not that we want to increase the resistance on the heart because ventricular hypertrophy is a thing often with devastating consequences to the electrical system). Therefore, HIIT is considered an effective training method vs. endurance cardio.
- Take care of your electrical system by replenishing electrolytes that are lost in sweat.
In the references and resources, I’ve included some videos that provide a much more comprehensive explanation of the cardiac cycles down to the cellular level. Please consider reviewing them to further your understanding of the cellular activities of the heart!
References:
VIDEO: Action Potentials in Cardiomyocetes
https://www.khanacademy.org/science/health-and-medicine/circulatory-system/heart-depolarization/v/action-potentials-in-cardiac-myocytes
The Clinical Significance of the Atrial Kick:
https://academic.oup.com/qjmed/article/111/8/569/4994786
Cardiophysiology Study Sheet from Kansas University Medical Center
www.kumc.edu/AMA-MSS/Study/phys2.htm
New England Emergency Medical Services explanation of Cardiac Muscle







