Because the symptoms of Chronic Fatigue Syndrome, or myalgic encephalomyelitis (ME/CFS), can be exacerbated by exertion, there are key points every personal trainer can keep in mind in order to better serve clients who may be sufferers.
Some of our clients may experience abnormal fatigue as excess baggage, thereby impacting their capacity and capability to train effectively and regain bodily homeostasis.
Besides learning to face and deal with fatigue during a workout this article aims to:
- Cite timeless aspects of these fatigues that we face.
- Differentiate between “normal” fatigue and chronic (abnormal) fatigue, then offer nervous, physical, and mental warning signs or symptoms for awareness.
- Describe abnormal fatigue as a symptom of underlying conditions or even diseases that trainers should be aware of and should practically accommodate.
- Consider viable energy boosts and lifestyle changes.
Fatigue wasn’t born yesterday!
Ancients defined fatigue as “ satiety or surfeit”. This term evolved to mean “tire out” and then to mean, “a task that causes weariness.”
Roman stoics encouraged proteges to exercise until weary, then return to their even-keeled, scholarly ways. They truly appreciated the linkage among the brain, nerves, and muscles to maintain balance, or homeostasis, in life. One stoic, Epictetus, encouraged Romans to acknowledge a split between what factors in life can be influenced or controlled, and what cannot.
With this conscious split in mind, consider this training scenario:
A middle-aged client shares a general malaise with their trainer and is frustrated for not being in control of personal progress from training progressions.
Has this client lost the ability to influence or control progress?
A short answer is that it depends.
[sc name=”stretching” ]
Differentiating Exercise Fatigue and Chronic FATIGUE
- fatigue: Exercise-induced tiredness or short-term lifestyle weariness is the type of “normal” fatigue that clients and their trainers can favorably influence with energetic activity and prudent rest. Think of overtraining, excess caffeine, or burning the candle at both ends.
- With timing in mind, restorative rest and energetic activity should alleviate a client’s normal fatigue in a few days or weeks.
- FATIGUE: Conversely, chronic long-term fatigue, may have root causes that are not easily influenced by training. In fact, chronic fatigue may, unfortunately, be worsened by physical or mental activity, and may not improve with rest.
- Think of a client with cancer or rheumatoid arthritis (RA). Think of mental anxiety or depression. Or, think of chronic fatigue syndrome which is not directly related to disease or medical condition.
- When weariness or fatigue extends beyond several weeks, then the client and trainer may, unfortunately, be facing abnormal or chronic fatigue. It is then a probable time for medical professionals to get involved.
- Think of a client with cancer or rheumatoid arthritis (RA). Think of mental anxiety or depression. Or, think of chronic fatigue syndrome which is not directly related to disease or medical condition.
Trainers should be aware of common warning signs of abnormal or chronic fatigue. Some of these cautionary signs may be manageable and others may not be:
- Medications
- Recent medical treatments, or surgical recovery
- Infections
- Chronic diseases like diabetes, heart disease, kidney disease, liver disease, thyroid disease, and chronic obstructive pulmonary disease (COPD)
- Fibromyalgia
- Anemia
- Sleep apnea.
[sc name=”cancer” ]
Chronic Fatigue Syndrome
ME/CFS is a serious chronic condition that affects the body systemically (CDC, 2018). Individuals who suffer from this disease face extreme challenges in performing normal everyday activities. Ultimately, their quality of life diminishes as they battle a myriad of symptoms.
Over 800,000 individuals suffer from ME/CFS and about 90 percent have not been diagnosed (IOM, 2015). It’s possible one or more of your fitness clients fit into this category. While it is not within the scope of practice of a fitness professional to diagnose any condition, it is our responsibility to understand special populations and the impact exercise has on certain conditions.
Symptoms of Chronic Fatigue Syndrome
Knowing what to look for and what questions to ask about potential symptoms outside of a training session is a great place to start with a client who has been diagnosed. Even without a diagnosis, familiarizing yourself with the following symptoms may alert you to refer your client who may be suffering from ME/CFS:
- Sleep disturbances. Individuals who experience ME/CFS may not ever feel rested even after a full night of quality sleep.
- Cognitive processing and memory issues.
- Orthostatic intolerance. ME/CFS sufferers often experience dizziness, weakness, and lightheadedness that may worsen upon standing or sitting up.
- Worsening of symptoms after mental or physical activity. This is referred to as post-exertional malaise (PEM).
- A significant drop in the person’s ability to perform normal activities prior to the illness lasting six months or longer.
- Extreme fatigue that is not a result of unusually difficult activity, is not relieved by sleep or rest, and has not been lifelong.
- Muscle aches and pains.
- Tender lymph nodes.
- Digestive issues.
- Chills or night sweats.
- Headaches – new or worsening.
(ACE, 2014; CDC, 2018)
When working with fitness clients, monitoring long-term health is equally as important as the pre-exercise screening process. Continually check in with clients to note any gradual or alarming changes in their health status or anecdotal comments. If you suspect something gravely concerning is occurring, refer the client to his or her primary care provider for further examination.
Difficult to Diagnose
Chronic Fatigue Syndrome isn’t an obvious condition and is challenging to pinpoint. Doctors must rule out a number of other potential illnesses and cause for the symptoms before a diagnosis can be reached. Consequently, achieving a diagnosis of ME/CFS can be arduous and time-consuming (ACE, 2014; CDC, 2018).
How Exercise Impacts Chronic Fatigue Syndrome
For those who experience ME/CFS, the symptoms aren’t just obnoxious, they are crippling. Exercise doesn’t seem to be a relief or treatment as was once believed. Previous information about this condition has perpetuated a misconception that exercise is a way out of the confines of ME/CFS (Science Daily, 2017). The disease itself was previously believed to be rooted psychological influences, which has since been discredited (Wessely, David, Butler, & Chalder, 1989; Science Daily, 2017).
In other words, encouraging chronic fatigue patients to engage in exercise was believed to be an effective treatment. Research now tells us that is no longer the case. Here’s what you need to know as a fitness professional:
- More exercise is not better nor does it lessen the impact of the disease.
- Activity can worsen the symptoms and cause Post-Exertional Malaise (PEM), thus magnifying the fatigue associated with the disease.
- Exercise should be done in conjunction with doctor’s supervision
- The goal of any activity should be to improve the quality of life of the ME/CFS individual rather than being performance focused.
(ACE, 2014; Science Daily, 2017).
Energy Boosts or Lifestyle Changes
Acknowledging the complexities of fatigue factors, professional trainers may need the support of medical professionals to evaluate proper volume, intensity, and tempo of energetic workouts for clients. For some cancer survivors, exercise may or may not be recommended.
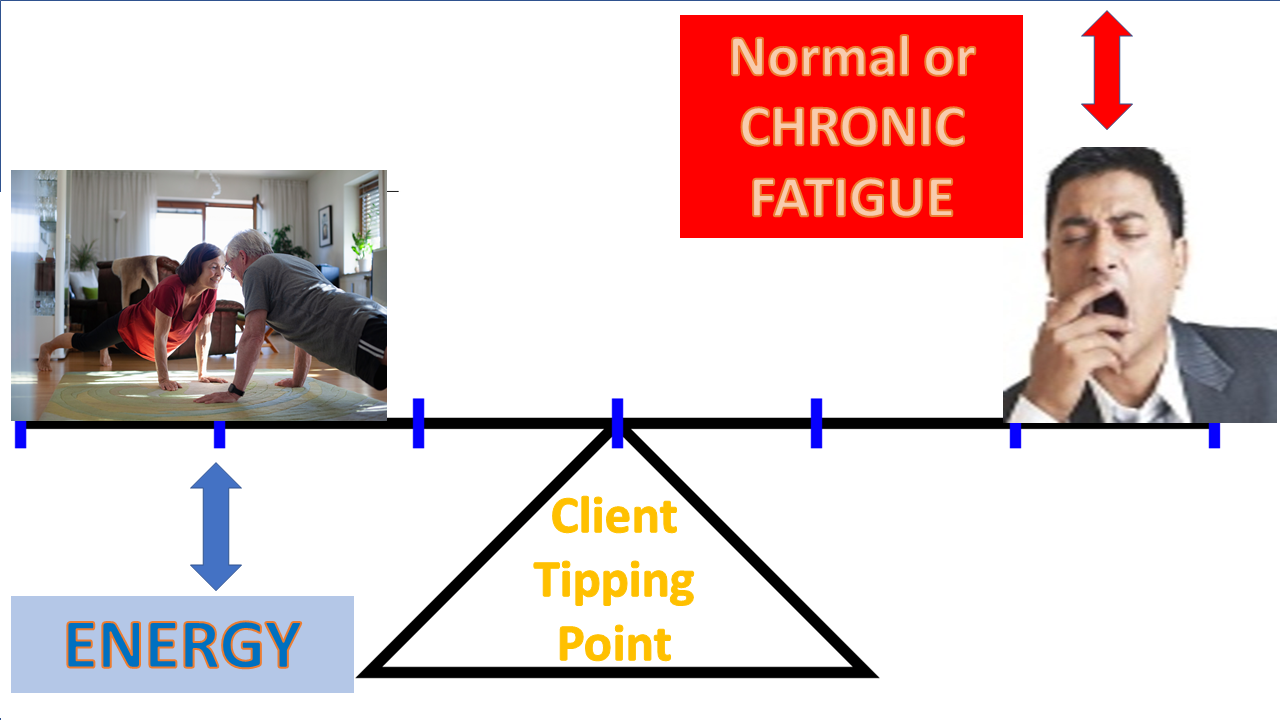
The see-saw depicted earlier suggests that applied energy may, or may not counter-act the complexities of fatigue.
When facing this dynamic see-saw, a trainer may consider and possibly suggest:
- A journal to document fatigue patterns
- Breathing and balance activities
- Avoidance of long afternoon naps
- Moderation and timing of alcoholic drinks
- An adjustment for the timing of daily activities
- A new evaluation of daily energy equations (macro-nutrient consumption vs caloric output).
Because the guidelines previously associated with managing and treating ME/CFS are being updated and new research is being conducted, there are no specific “do this or don’t do that rules” that help fitness professionals or patients with the condition navigate its complexity. As more research is released, this is likely to change.
For now, personal trainers can work with a chronic fatigue patient’s physician to create a balanced plan that doesn’t exacerbate the fatigue or worse the symptoms. Try approaching any activity with a “less is more” perspective.
Here are some ideas to try/suggest:
If symptoms worsen or become exaggerated, clients are encouraged to return to the most recent manageable level of physical activity tolerated (ACE, 2014).
Potential Cause and Cure For Chronic Fatigue Syndrome?
American researchers believe they had found a link between xenotropic murine leukemia virus-related virus (XMRV) and CFS. If that proves to be true, scientists could begin working on effectively diagnosing and treating the disease.
The results of the study were published in the journal Science in an article entitled “Detection of an Infectious Retrovirus, XMRV, in Blood Cells of Patients with Chronic Fatigue Syndrome.” Researchers sought to determine if there was a connection between a pathogen and CFS after observing that many people develop CFS after a bout with a flu-like illness. The new study compared samples of blood from 101 people with chronic fatigue to samples from 218 healthy people. Approximately 67 percent of those ill showed the presence of XMRV, compared with fewer than 4 percent of healthy people.
Researchers have suspected for some time that chronic fatigue might be caused by a virus. In the late 19th century, American neurologist Dr. George Beard applied the term neurasthenia to a range of symptoms. Since then, the medical community has been unsure whether the condition is a physiological or a psychological condition. It wasn’t until 1988 that the name “chronic fatigue syndrome” was offered by researchers at the CDC.
While most viruses are eliminated from the body, XMRV belongs to a separate class known as retroviruses: they linger on in the body indefinitely. Some retroviruses are known to infect immune cells. XMRV has also been found in some prostate tumors in humans and is related to a retrovirus that causes cancer in animals.
Scientists also say it’s too soon to say whether XMRV actually causes chronic fatigue. In the past, some of the other supposed causes of CFS have included enteroviruses, the Epstein-Barr virus, and the herpes virus. However, these have been found in a smaller percentage of CFS cases than XMRV.
ME/CFS is still a mysterious disease that the medical world has not yet been able to solve or cure. It’s frustrating and debilitating to those who are afflicted by it. Fitness professionals have a responsibility to monitor client progress and determine when a referral is necessary. If you currently have clients suffering from a diagnosed case of ME/CFS, work closely with the client’s physician in order to determine the best course of action.
References
ACE (2014). ACE Personal Trainer Manual, 5thEdition. San Diego, CA: ACE
https://www.cdc.gov/me-cfs/about/index.html
http://www.nationalacademies.org/hmd/Reports/2015/ME-CFS.aspx
University of Florida. (2015, March 12). Why exercise magnifies exhaustion for chronic fatigue syndrome patients. ScienceDaily. Retrieved February 19, 2019 from
www.sciencedaily.com/releases/2015/03/150312154135.htm
Wessely, S., David, A., Butler, S., & Chalder, T. (1989). Management of chronic (post-viral) fatigue syndrome. Journal of the Royal College of General Practitioners.Retrieved February 20, 2019 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1711569/pdf/jroyalcgprac00001-0034.pdf
“Detection of an Infectious Retrovirus, XMRV, in Blood Cells of Patients with Chronic Fatigue Syndrome.” Vincent C. Lombardi, et al. Science. October 8, 2009.
Additional Author: