Working with a client who is a cancer survivor? There is a good chance they may have brittle bones. To create safe and effective exercise programming you need to know if there has been an osteoporosis diagnosis.
Those of you who have taken the NFPT Cancer Recovery course know that surgery, chemotherapy, radiation, and hormonal therapy have side effects, which exacerbate the problems faced by cancer patients.
Surgery can create adhesions that can limit range of motion, and cause pain, numbness, and tightness. Removal of lymph nodes creates scars and may decrease range of motion and lead to lymphedema.
Chemotherapy may affect balance, a patient’s immune system, and cause nausea, light-headedness, vertigo, neuropathy, fatigue, sarcopenia (loss of muscle mass), and anemia.
Radiation can cause fatigue, tightness, and stiffness. Hormonal therapy can cause joint pain and early menopause and the side effects associated with menopause. Surgery, chemotherapy, and radiation can also increase the risk of developing osteoporosis.
Cancer surgery and treatments affect the entire body, not just the area of cancer. Everyone has different reactions to the treatments. Sometimes the effects become apparent after the treatment is finished. Some symptoms can appear years later.
Among the problems associated with cancer is an increased risk for osteoporosis or bone loss that increases the risk of fracture. Breast cancer and prostate cancer patients need to be made aware of their increased risk of osteoporosis and told what they can do to decrease their risk.

Osteoporosis means porous bone and is a chronic disease that weakens the bones. It is a serious health issue. With osteoporosis, bone density decreases and the bones become fragile and break easily.
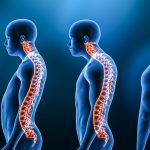
Although it can cause a break in any bone, the most common sites for breaks are the hips, spine, and wrist. A broken hip or spine usually requires a hospital stay or surgery and can lead to permanent pain, disability, or death.
Bone loss occurs in everyone, as we get older. The leading causes of osteoporosis are decreased estrogen in women at menopause and lowered testosterone levels in men. Bones loss speeds up during and after menopause as the protective effect of estrogen in the body declines. In fact, a woman can lose about 20 percent of her bone mass in the five to seven years after menopause.
The most common breast cancer is estrogen based. Cancer treatments work by starving the cancer of estrogen. The combination of the high incidence of breast cancer together with increased survival rates will increase the percentage of those suffering from breast cancer and osteoporosis.
The following cancer treatments can lead to a loss of bone density:
1. Aromatase Inhibitors
Aromatase inhibitors are used in post-menopausal women diagnosed with hormone receptor positive cancer. In post-menopausal women, aromatase inhibitor agents to reduce the risks of cancer recurrence result in decreased estrogen and cause an increase risk of osteopenia/osteoporosis and fractures.
Aromatase inhibitors inhibit aromatase from turning androgen into estrogen in other parts of the body besides the ovaries.
The aromatase inhibitors are: anastrozole (Arimidex), letrozole (Femara), and exemestane (Aromasin)
2. Androgen Deprivation Therapy
Androgen Deprivation Therapy hormone therapy leads to numerous side effects, which can be decreased through exercise. The side effects of ADT include loss of muscle, increase in fat mass and osteoporosis. A patient’s risk for diabetes and heart disease also increases. Men with prostate cancer who receive androgen deprivation therapy risk loss of bone density and fractures.
3. Chemotherapies
Chemotherapy has a major effect on bone health by shutting down the ovaries and causing early menopause in premenopausal women. The decreased estrogen state has a negative impact on bone density. Doxorubicin (Adriamycin), methotrexate (Trexall), cyclophosphamide (Cytoxan) and 5-fluorouracil can cause premature menopause.
4. Oophorectomy
The surgical removal of the ovaries will induce an early menopause.
5. Medically shutting down the ovaries
Used for hormone-receptor-positive breast cancer. Shutting down the ovaries decreases estrogen, in order to decrease cancer growth. Unfortunately, this leads to lower bone density, especially if the ovaries are shut down at an early age.
6. Use of corticosteroids
Some medications used to prevent nausea and vomiting may also have a negative impact on bone health.
7. Sedentary lifestyle due to cancer fatigue
In addition to cancer survivors being at high risk for osteoporosis due to chemotherapy and cancer medications, balance issues are common. Balance can suffer after surgical procedures and treatments. Poor balance is of particular concern to those with brittle bones.
Falls and fall-related injuries, such as a hip fracture, can have serious consequences. Balance and strength exercises can help prevent falls by improving the ability to control and maintain body position whether in motion or stationary.
For those that are working with clients who have had TRAM flap reconstruction, be aware of balance issues because the rectus abdominus is altered. Poor core strength, caused by the change in placement of the rectus abdominus, has a negative effect on balance.
After a TRAM flap operation, it is necessary to learn how to compensate for this change of muscle placement through a series of exercises designed to strengthen the remaining muscles such as the obliques. Balance exercises can counter some of the effects of muscle imbalances and body asymmetry after surgery.
Some of the chemotherapies can affect balance. Neuropathy, a common side effect of chemotherapy, can make the feet numb and affect balance.
Fear of falling and fracturing might cause one to withdraw from daily activities and decrease quality of life. Stability exercises can help to enhance both steadiness and leg strength. Balance exercises will help one regain function and mobility for activities of daily living and are a key component for recovery after cancer treatments.
Bone loss is a common finding in patients with breast and prostate cancer. Prevention of osteoporosis is key and exercise, diet, and lifestyle changes should be emphasized to help prevent bone loss. Osteoporosis is typically less prevalent in people who are active, and exercise may also prevent osteopenia from becoming osteoporosis.
Proper body mechanics and form should be used throughout the day and during exercise sessions that include strength training, weight-bearing, stress reduction, posture, and balance exercises.
[info type=”facebook”]Join the conversation on the NFPT Facebook Community Group.[/info]