Concussion awareness and education are crucial for saving the life of clients who may not even be aware they have suffered one. A concussion can happen to anyone at any stage of their life who takes a fall. The populations most at risk are youth, athletes, and seniors.
Knowing how a concussion occurs and recognizing the signs and symptoms can help your client get a proper diagnosis from their physician, and knowing how to ease them back to normal activity can help them recover from this often under-recognized and underreported condition.
How does a concussion happen?
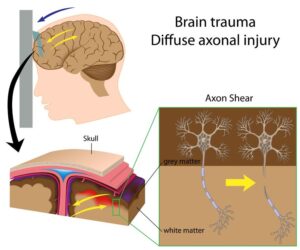
When a person receives a blow to their head, or an impact to their body that causes the head to snap back, the brain slams against the inside of the skull. Almost like Jell-O, brain tissue has the ability to stretch and reform its original shape.
This stretching can damage the axons of the neurons in the brain, causing them to tear or break. Axons send nerve signals from one neuron to another.
In the brain, the axons are bundled together. When the tissue is stretched, individual axons in an axon bundle can snap, like a rope beginning to fray.
This fraying effect causes an unwanted release of neurotransmitters resulting in a chemical imbalance in the brain, a disruption in normal nerve signaling, and inflammation of the brain tissue.
Signs and Symptoms of Concussion
Symptoms may not reveal themselves all at once. They can manifest over time. Symptoms of concussion include, but are not limited to:
- headache, pressure in head, nausea, difficulty breathing, numbness, tingling, neck pain, ringing in ears, sensitivity to noise, vomiting, fatigue, drowsiness, sleep disturbances, sleeping more than usual, difficulty concentrating, brain fog, difficulty remembering, dizziness, near-fainting upon standing, feeling dazed, poor balance, sensitivity to light, blurred vision, double vision, sadness, depression, irritability, being overly emotional, nervousness, anxiety, impaired fine motor function.
Rates of Concussion
In 2012 nearly 3 million concussions were reported in hospitals or emergency rooms in the US, however, the American Medical Society for Sports Medicine estimates that as many as fifty percent of concussions are not reported.
In 2013, 1 in 45 seniors age 75 and older suffered a head injury that resulted in an ER visit, hospitalization, or death. This rate of injury for seniors increased seventy-six percent from 2007 to 2013. Sixty percent of head injuries for this age group were the result of falls.
As the baby-boomer generation continues to age, these rates are expected to continue to increase. Many older adults do not seek the medical attention they need after experiencing a fall where they hit their head, fearing that they may be forced to give up living independently. However, this puts them at greater risk for subsequent concussions from a second or third fall.
Second-Impact Syndrome
If a person suffers a second concussion before recovering from their initial concussion, second impact syndrome can occur. The brain swells rapidly and catastrophically, creating an enormous amount of pressure inside the skull.
This pressure can compromise the function of the brainstem, leading to collapse, coma, and death. The time from the second trauma to failure of the brainstem can range from 2-5 minutes. This condition almost always results in death or permanent disability.
Physician Referral
If your client is experiencing symptoms consistent with a concussion, ask them if they have recently fallen or been knocked down, hit their head, or have been jarred violently (such as a car accident). If they answer yes, it is appropriate to end the session and refer them to their physician for evaluation and request they bring a note for clearance to return to exercise.
Return to Exercise After a Concussion
After a diagnosis of concussion, the best remedy is complete mental and physical rest. Upon physician clearance to return to exercise, it is important to avoid vigorous effort until all symptoms have fully resolved.
While exercise has been shown to improve the rate of recovery from a concussion, high intensity or high effort activity has been shown to prolong the recovery period because of the stress placed on the central nervous system.
How to Progress From Concussion Recovery
As your client recovers, you can increase the intensity of the workouts. The best way to approach their programming is to treat them as a brand new client who is very deconditioned. This is an excellent time to focus on technique, corrective exercises, and creating a better mind-muscle connection.
- Week 1 – Stability, mobility, balance, and bodyweight or low-intensity TRX movements
- Week 2 – Stability, mobility, advanced balance, bodyweight or TRX, and weight training
- Week 3 – If all symptoms have resolved, return to normal training and re-introduce higher intensity exercise
If symptoms persist or worsen, refer your client back to their physician for further evaluation.
Concussion Prevention
While it’s nearly impossible to prevent a concussion when kids are playing or during the heat of competition in sport, it is possible to reduce the likelihood of concussions in older adults by reducing their fall risk.
Baby boomers are living longer, and the senior population will continue to grow and need fitness professionals to help them live with vitality in their golden years. Incorporating lower body strength, balance, and agility training will reduce your senior clients’ risk of falling, and keep your sessions functional and fun.
As trainers, we strive to help our clients achieve their goals as well as better health and fitness outcomes by both incorporating exercises they enjoy as well as the exercises they need.
[info type=”facebook”]Join the conversation on the NFPT Facebook Community Group.[/info]
References
- What Is a Concussion? (2017, January 31). Retrieved from https://www.cdc.gov/headsup/basics/concussion_whatis.html
- Giza, C. C., & Hovda, D. A. (2014). The New Neurometabolic Cascade of Concussion. Neurosurgery, 75(0 4), S24–S33. http://doi.org/10.1227/NEU.0000000000000505
- Traumatic Brain Injury–Related Emergency Department Visits, Hospitalizations, and Deaths — United States, 2007 and 2013. (2017, June 21). Retrieved from https://www.cdc.gov/mmwr/volumes/66/ss/ss6609a1.htm
- Harmon, Kimberly G., et al. (2013, January). American Medical Society for Sports Medicine position statement: Concussion in sport. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/23269325
- Filer, W., & Harris, M. (2015, April 01). Falls and Traumatic Brain Injury Among Older Adults. Retrieved from www.ncmedicaljournal.com/content/76/2/111.full
- University of Washington Medicine (n.d.). Second-impact Syndrome. Retrieved from www.uwmedicine.org/health-library/pages/second-impact-syndrome.aspx
- Recovery from Concussion. (2017, June 26). Retrieved from https://www.cdc.gov/headsup/basics/concussion_recovery.html
- Lal, A., Kolakowsky-Hayner, S. A., Ghajar, J., & Balamane, M. (2018, March). The Effect of Physical Exercise After a Concussion: A Systematic Review and Meta-analysis. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/28570092
- Chung, J. P., Lee, J. H., Howell, D. R., Meehan, 3. R., Iverson, G. L., & Gardner, A. J. (n.d.). Effects of Exercise on Sport Concussion Assessment Tool-Third Edition Performance in Women. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/30015637